To evaluate skin pigmentation in different skin layers, a special light adapter is needed to take multispectral pictures of the skin. As there are different optical properties of skin pigments, four different light sources have been chosen.
- blue λ= 470 nm – highly absorbed by epidermal melanin
- green λ= 576 nm – hemoglobin peak
- red λ= 660nm – epidermal-dermal boundary
- IR λ= 865 nm – low absorption, sensitive to scattering to measure papillary dermis thickness.
There was a lighting source for the “Nikon Coolpix E3100” digital camera developed to take multispectral images of skin.
Making an adapter
The drawing of lighting adapter
The lightning adapter isn’t tough to build. It would help if you made a circular PCB and solder LEDs with protective resistors. The PCB image:
PCB Mask
REAL view
Then soldered LEDs symmetrically to distribute the smooth light:
LED’s are in a row: Red, Green, Blue, and IR, White. White LED is optional to make normal pictures of skin.
Then I made a hole for camera optics. It also serves as the holder of PCB. As you see in LEDs, I put a polarizing filter (another is placed on optics of camera with polarization axis crossed to this one). This filter is used to filter light reflections from the surface layer of skin to remove flares. Then you get the image of deeper skin structure.
The beautiful shiny LEDs are working:
Testing an adapter on a skin
I had some problems to focus them on one spot. LEDs have not ideal characteristics, and they weren’t ideally soldered to board. You can see my effort 🙂
I only needed one square centimeter of the region to be smooth lightened.
The finished adapter:
About skin reflectance modeling, there are other topics created, and you’re welcome to read them. There I will put a few impressive results about taking photos of skin and lesions.
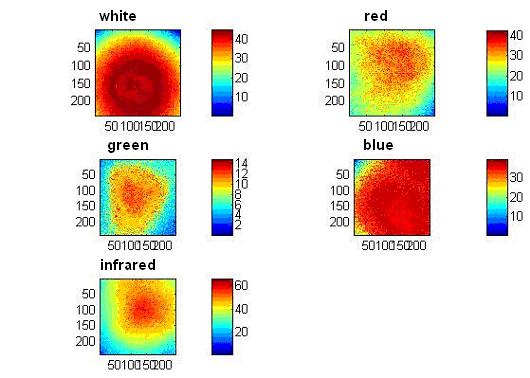
Here are the matrices calculated for each color. They are subtracted from every picture I made to suggest that lighting is equal to all points on the 1x1cm region:
Let’s make some test shots:
Benign lesion:
First test results
I didn’t make Infrared here, as this lesion is benign and doesn’t show any skin structure changes.
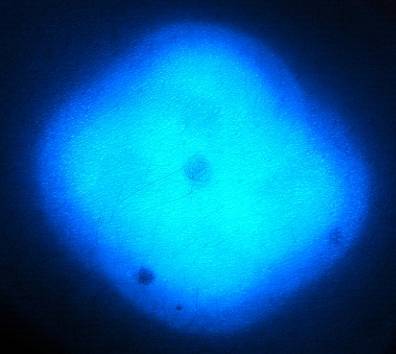
Suspicious lesion as you can see Infrared (fig e) picture shows the view from deeper skin layers:
And here you can see parametric maps generated using a model with these images:
Here are images with hair and benign lesion:
As this light adapter is hand made and calibration is weak, there can still be good results. This experiment proved that a handheld digital camera and simple lighting adapter could show relative diagnostic results while inspecting skin lesions.


























I have seen a similar DIY project before that combines a lens/light system with a piece of software that tracks location on the body of moles. Are you BJones?
Very interesting. If this was made by HP or Physio-Control it would cost $100,000
Try putting a diffusion filter (common shirt-box tissue paper works well) between the LEDs and the second polarizer to evenly blend the light and flatten the illumination. Question: How do you arrive at results that are diagnosticly meaningful? You mention creating parametric maps, but don’t say how. Very cool idea, especially if the final steps to interpreting the images and determining a positive result can be performed easily!
this is a very very good little gadjet you made great job keep up this great work i love doing stuff like this
omg you rule, i been looking to make something like this thank you!
Well, I guess that is some sort of bullshit. The only real difference us visible under IR. The calculation you did, although using Matlab, about “hemoglobin” and “melanin” is complete nonsens. All these substances do not only absorb at theyr special wavelength but do also at different wavelengths. Thats why inferring from these pictures physiological states is bs. The only thing that has some merrit to it is the IR thing, but come on, no doctor would rely on such subjective measurements. Just taking a look and later a biopsy is the usual way and it is a good way.
There were a request of chematic of this adapter. I’ll publish it soon, as there is nothing tricky. Thank you.
Wow I didn’t think there are so many of you interested in this matter. I guess I will have to publish more of this. I just want to warn you, that I am not a doctor, but biomedical engineer so my view is little different from doctor’s. But this issue were interesting to me as well and there is much more to investigate in this field.
Great job! I’ve done a bit of optics work, and am amazed by what you have achieved with relatively simple components.
There is a little trick that I’ve used for non (spatially) uniform sensors, that may help in your case of non uniform (spatially) illumination: Obtain calibration images with each of the different wavelengths, using a specular white surface, then use these calibration images to correct for the non-uniform illumination in software. You will need to have a registration mark of some kind, or make sure that the rotation of the device on the camera is repeated between the calibration images and the actual images. The software is pretty simple, just correct each pixel with a multiplier that is the inverse of the intensity of the pixel in the calibration image – so the value across the region of interest would then be constant for a calibration image, after the correction is made.
Wow… I didint even knew how this kind of equipment worked… (Or even existed….) very interesting job….
My whole congrats!!!
Thanks much for this page. I’m very interested in this topic, as my fiancee has some issues with skin cancer. She’s had two suspicious lesions removed, and although she’s in good health otherwise, this is a worry. Can you provide more information regarding the actual items used? Does the lighting require very specific wavelengths and intensity of light? Did you also create a controller to turn on/off colors one at a time, or did you use software to filter?
Thanks much!
Your a frickin genius.
/What is the mcd output of the LEDs you used?/
I was using relative values, I did not tie to absolute I can only provide manufacturers characteristics of leds.
A google scholar search (melanoma infrared) turns up more on the research into similar devices, for those who are interested in digging deeper.
Cool that you were able to make a useful device almost entirely from cheap and easily available parts.
That’s great, but all of that work could have been simplified by channel mixing a digital shot of the same target in full spectrum sunlight.
You can get the same effect with a high-res digital shot channel mixed in photoshop….a lot les soldering.
Entertaining work, though.
You can get the same effect with a high-res digital shot channel mixed in photoshop….a lot les soldering.
Entertaining work, though.
What is the mcd output of the LEDs you used?
um, it already exists and has for quite some time:
http://www.dermlite.com/dl2ms.html
And how do you DEFINE melanoma? What about atypical nevi? What about Spitz nevi? What about Pigmented Spindle Cell nevus of Reed? Can it tell these apart? Lentigo Maligna? What about amelanotic melanoma? Tell me what you MEAN by melanoma.
Personally me, I cannot define melanoma or other types of lesions. My method is only showing the relative distribution of pigments in skin layers. Presence of melanin in dermis doesn’t show that it is melanoma or Spindle Cell nevus or Spitz nevi. There are so many factors who define lesion type: melanin spreading shape inside dermis, blood behavior inside lesion and around it, the thickness of collagen layer in papillary dermis. As i don’t have qualification for this, I just can do a math and nothing more. And it needs much More investigations to be done to use this method of visualisation. This tool i made just can be a tool to dermatologist to see more inside the structure of formation of lesions, but it doesn’t show is it a melanoma or other type of formation. Very good question. Thank you.
The spectrum emitted by an LED is 25-50 nm wide. This is much narrower than the 150-200 nm bandwidth of the cones in the eye. I think the color filters in a color camera also have a relatively wide bandwidth, like the eye. So the LEDs offer a few times higher spectral resolution than is possible with white light alone, (short of using a spectrometer).
Also, there are a lot of combinations between 4 (or more) LED colors, and the RGB camera filters.
4! * 3! = 24 * 6 = 144 (note not all are useful) Simple software can process the pixel data arithmetically (yielding more color combinations), thus enhancing the resolution even further.
MM, I am a curator for an art/culture/science exhibition going on at Columbia College Chicago in March 2007. We would love to show this project as part of the exhibition. You can read more about the show at http://www.diychicago.org. If interested please get in touch. Many thanks.
i took a great peice of knowledge abt this from here and anow putting it up on myweb.
very interesting and informative article thankx for sharing.
Amazing work!!! Same question as the 4th comments: how do you make parametric maps from these images?
That is some piece of optical engineering masterpiece!
can
pls u upload video…